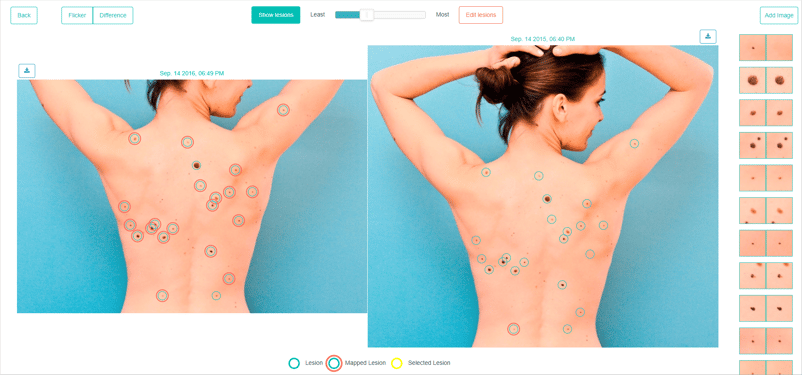
Total Body Photography: A Valid Approach For Improving Patient Care
Is there any evidence that mole mapping helps our patients — have there been any prospective, randomized controlled trials to show that mole mapping helps to detect malignant melanoma early and increases patient survival?
First, it is important to note that mole mapping is a medical record, not a therapy. The physician determines whether or not a lesion should be removed. This decision is based on multiple factors and total body photography provides an opportunity for the physician to incorporate an objective assessment of lesion change into the decision-making process. This is not unlike using the medical record to identify changes in laboratory values, EKGs or radiological studies. The appropriate question should be, “Do data on lesion change impact patient care?”
One aspect of patient care is melanoma detection. Melanomas result when the proliferation of melanocytic cells becomes uncontrolled. Thus, biologically, a growing melanocytic lesion should be considered worrisome for melanoma.
In a controlled study by Thomas et al evaluating the ABCDE criteria, “E” (enlargement) was the only statistically positive increasing feature that could differentiate melanomas from dysplastic nevi.2 In recent studies following concerning lesions with dermoscopy, melanomas have been found to increase in size, often in an asymmetric manner.3-5 With total body photography, non-uniform and growing lesions were found to be statistically more likely to be melanoma.6 There is therefore sufficient information to suggest that data on lesion change is important in melanoma detection.
Reducing BiopsiesA second important aspect of patient care is the reduction of unnecessary biopsies.
Annually, a large number of benign dysplastic (atypical) nevi are removed unnecessarily. In one paper advocating the removal of nevi with clinical signs of dysplasia as a mechanism to reduce melanoma risk, 136 benign lesions were removed for every melanoma in patients with a previous melanoma diagnosis; 577 benign lesions were removed for every melanoma in patients without a previous melanoma history.7
Biologically, a lesion that has stopped growing is unlikely to be malignant. In dermoscopy studies, lesion stability has been used to successfully differentiate between benign and malignant lesions.3,4
Clinicians who utilize total body photography in patient follow-up report relatively low benign/malignant ratios some at or below 3 to 1.8,9 Overall annual biopsy rates per total body imaging patient have been reported at approximately 0.15 and 0.08.6,8 These studies strongly suggest that data on lesion stability reduces unnecessary biopsies and associated morbidity.
A third important aspect of patient care is impact on survival. Since few patients with thin melanomas die, differences in survival data will be difficult to obtain. In melanoma vaccine trials, most do not even accept patients with thin melanomas due to the low likelihood of events. Almost all melanomas removed by physicians using full body imaging are thin.8,9 When compared to the community, tumors removed by physicians who incorporate total body photography into their practices tend to have thinner Breslow’s depths8 and thus there may be a survival advantage.
Increasing Patient Satisfaction
A fourth not well-quantified aspect of patient care is patient involvement, satisfaction, and reduction of anxiety with total body photography. It is my impression that patients given a copy of their photos feel more secure having data at their fingertips, feel more involved in their own care, have less anxiety, and are more satisfied with the data-based approach to follow-up.
As Dr. Goldenberg suggested in his article, the patient (or family member) often initially identifies the melanoma, so it is important that he or she have the full body imaging data on hand to use for confirmation of change.
In summary, data do exist detailing how mole mapping helps our patients. These data support “change” as the most important discriminator in melanoma detection, and lack of change as a critical determinate for avoiding unnecessary biopsies.
Total body photography medical records provide objective data on lesion change, it’s up to the physician and patient to determine if they want this information available when deciding whether a lesion should be removed.
The Issue of Cost
The cost of total body photography should be covered by a patient’s medical insurance. The new AMA CPT category I code status (96904) for full body imaging (defined as “whole body integumentary photography, for monitoring of high-risk patients with dysplastic nevus syndrome or a history of dysplastic nevi, or patients with a personal or familial history of melanoma”) validates the service, and the hope is that it will result in improved coverage.
Many insurance companies now cover MoleMap CD/total body photography services, and the trend has been very positive over the last few years. Covering total body imaging should be a win/win for the insurance companies if done properly. If used appropriately, it will markedly reduce unnecessary biopsies while allowing the detection of thin melanomas.
At Duke, the cost of a punch excision, surgical tray, pathology processing, and professional fees easily exceeds $500. The cost of a MoleMapCD is $395. Thus, if total body photography eliminates the need for one biopsy, it pays for itself and will build additional value by continuing to spare the patient future unnecessary biopsies and/or excisions.
In order to gain the greatest potential from full body imaging, it should be used primarily on patients most likely to have numerous biopsies. This includes patients with dysplastic nevi, especially those with a personal or family history of melanoma and highly anxious melanoma patients worried about every skin lesion.
Documented lesion stability gained through comparison with an established baseline can prevent most unnecessary biopsies. However, particularly in children and young adults, be aware that acquired nevi also have a growth phase, so it is important that the physician be comfortable with incorporating other features in addition to growth in determining whether a lesion needs to be removed. This is best done by first examining a patient from from head to toe, identifying unusual moles (those that are clinically different from other moles identified by the patients or dermoscopically, not a clearly benign pattern), and then determining whether they have changed.
An unusual and changed mole should be considered for excision; if non-uniform features6 are also present, then the concern about melanoma is further increased.
The highest efficiency will be obtained when total body photography is used by physicians comfortable with the process of sorting out benign from malignant lesions by incorporating growth changes with other features in their decision-making process.
Benefits for Patients, Physicians and Insurers
In order for total body imaging medical records to garner the most benefit for insurers, physicians and patients, they need to include high-quality images of the entire skin surface at sufficient resolution to be able to detect lesion changes. The programs should be consistent, easy to use, and clinically efficient.
There are currently two approaches to total body photography — a physician-supervised in-house approach (requires physicians to have their own equipment, designated permanent space and trained staff) and an outpatient full body imaging service (handles scheduling, imaging, quality assurance, billing, and provides a standardized total body photography record at no cost to the physician). In either case, physicians, patients and insurance companies must require that total body imaging records be of high quality, transferable and easily used by patients and physicians.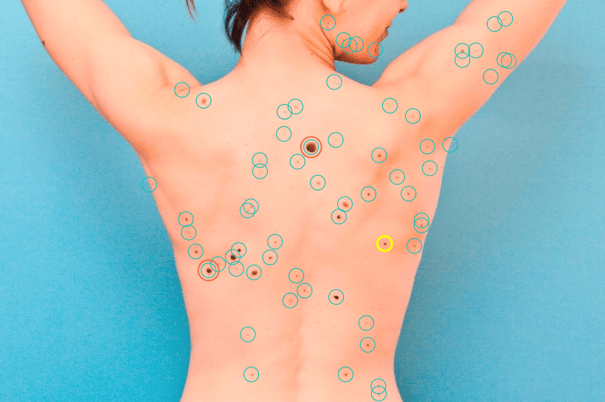
Again, the cost of total body imaging should be covered by the patient’s medical insurance. Those with top- quality insurance products will probably receive coverage, but others will have to decide if total body imaging is worth the out-of-pocket costs. However, this out-of-pocket approach lets insurers “off the hook” and diminishes the importance of total body photography in the melanoma detection process.
If you feel full body imaging is the correct avenue of documentation for your patient, communicate that message to the patient and to the insurance companies. Perhaps then, in the near future, insurance coverage for total body photography will no longer be an issue.
Answering Medical-Legal Questions
The objective of total body photography is to help the physician and patient identify early melanomas and avoid unnecessary biopsies. The patient is included in this process and should be educated and given a copy of the images for home use. Total body imaging documents the patient’s baseline examination. Clearly, some patients are difficult and may have numerous worrisome lesions.
On the initial examination, use your best judgment and remove any lesion clearly worrisome for melanoma. Melanomas change, and it is this change that will help in the identification of the melanoma at a follow-up visit. Almost uniformly these melanomas are still at very early stages of development.
It has been my experience that most melanomas arise in normal-appearing skin, and when a lesion was present at baseline, it appears similar to multiple other lesions documented on the patient’s skin surface. When a lesion is selected for excision, the area should also be photographed to document the change.
Patients who are engaged with their own care, in part by having a copy of their total body photos, appreciate that melanoma detection is not easy and is a shared effort.
Certainly there will be cases in the future that may be won or lost, but in the high-risk melanoma arena, I’d rather go into court with high-quality total body photography data documenting the patient’s skin surface at baseline and the follow-up image demonstrating the change (that allowed identification) than to hope that lack of documentation will be taken by the jury as proof I didn’t make a mistake.
Standard of Care?
The term “standard of care” has evolved to indicate a strictly black-or-white approach to patient care. For some, if it’s not standard of care, it should not be used, while if it is standard of care, it must be used at the risk of a lawsuit.
In the melanoma world, there has been significant pressure to define sentinel node biopsy (SNB) as standard of care despite the lack of survival benefit10 and the huge costs (approximately $1,000,000 in patients with melanomas less than 1.2 mm to detect one patient with a positive node11).
The SNB issues have made many of us worry that once something is dubbed “standard of care,” we have no choice in the matter, but medical care should not be black or white. Personally, after using total body photography in my clinic for more than a decade, I cannot imagine how I could handle many of these “moley” and/or highly anxious patients without it. At the same time, there are patients I feel comfortable following without total body imaging.
Total body photography correctly used on the right patient population will save money, reduce unnecessary biopsies, decrease morbidity, and allow for the detection of melanomas at earlier stages. It is a well-established and valid approach to patient care. If we need to define it as standard of care in order for insurance companies to cover the costs, then it should be considered a “standard of care” for the correct patient.
Interested in seeing how DermEngine's total body photography tools are enhancing the practices of medical professionals around the world? sign up for a demo today!
Original article can be found at: https://www.the-dermatologist.com/article/6857
Topics: Dermoscopy Skin Cancer Total Body Photography Full Body Imaging