Top 5 Total Body Photography Breakthroughs Of 2019
Total body photography services have progressed immensely over the past decades- from projector slides, camera film, and floppy disks to digital imaging, mapping, and uploads. How is artificial intelligence (AI) driving changes we are only beginning to experience in 2019?
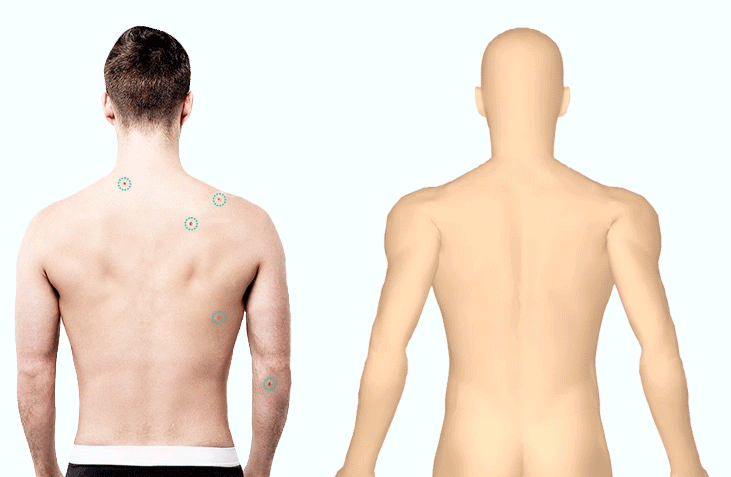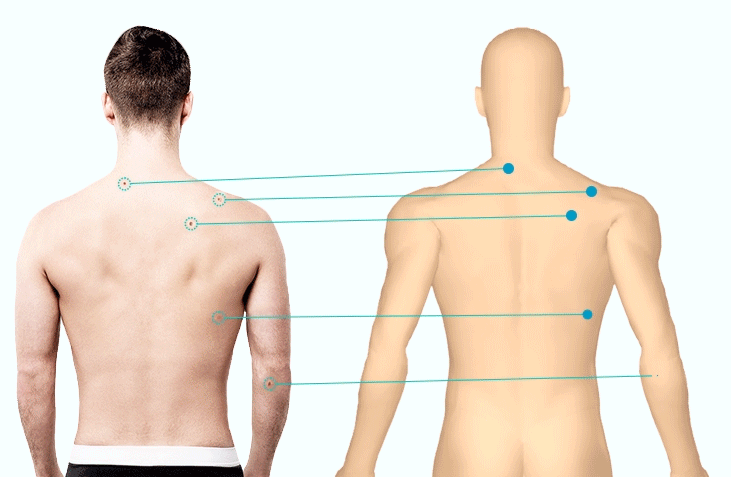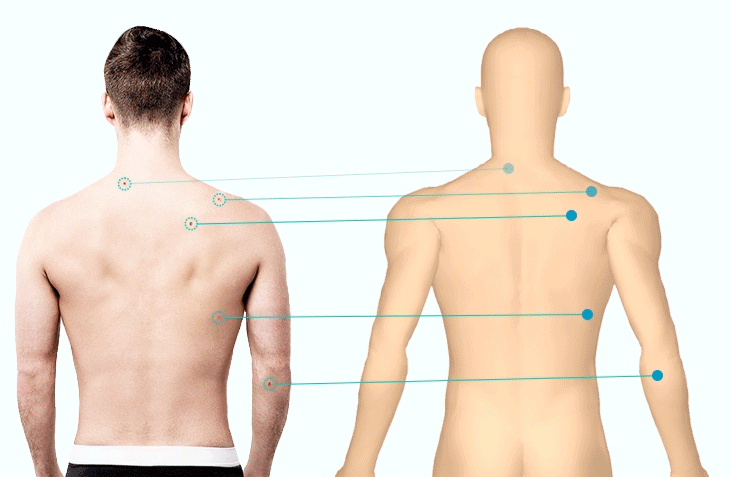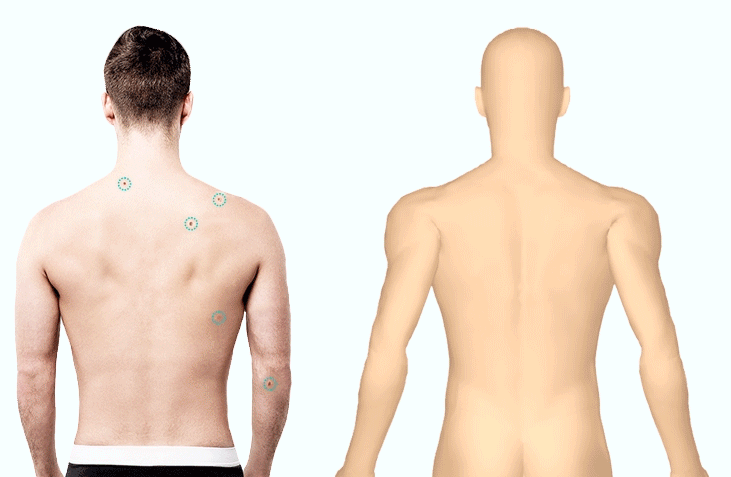
1. Lesion MappingThe first asset in a dermatologist’s toolbox, lesion mapping is the process of recording a patient’s skin spots on a paper diagram (traditional) or digital body map (modern). The challenges associated with this newer method is that it is still time-consuming to identify, map, and image all necessary spots. In spite of its efficacy for supporting dermatologists and other medical professionals in the early detection of skin cancer, this remains a large deterrent (alongside machinery costs).
To streamline workflows, intelligent algorithms have been developed that automatically identify all spots within an image and map them to the patient’s personal 3D Body Map. Research indicates that doctors dedicate nearly 50% of their work day to administrative tasks; rather than wasting minutes manually documenting spots (accumulating to lost hours each week) they can be mapped in seconds.1 Not only does this save valuable time within a medical professional’s day, it allows them to focus on what matters- their patients.
2. Lesion MatchingAnother challenge associated with total body photography is identifying subtle changes to the skin over time. Like finding a needle in a haystack, the dermatologist must dedicate all of their focus to combing over subsequent images to find potential causes for concern. Currently, this is achieved through comparing dermoscopic, overview or total body images next to one another. What happens when documents are misplaced, mislabeled, or simply unavailable? The most impactful portion of this imaging method can become its weakest- without a proper tracking system, total body photography loses its distinct advantage.
To combat this, an intelligent dermatology software has recently offered a new feature that compares the most recent image to previous ones while identifying any causes for concern which are automatically prioritized by amount of change for the medical professional’s convenience. Through utilizing this lesion matching tool, the dermatologist can combine their experience of lesion identification with powerful award-winning algorithms to enhance their ability to identify changes to spots over time and promote the early detection of skin cancer.
3. FlickerBuilding on this idea of smarter comparison solutions, Flicker takes a traditional comparison method and enhances it with artificial intelligence. When trying to identify changes to a patient's spots, you will likely place the two images side by side, or (if the images are somewhat transparent) overlay them clearly indicate any evolutions. Rather than waste time squinting between the two pictures, the Flicker tool overlays the two total body images and “flickers” between them to show any changes over time more clearly so dermatologists can review images with a greater level of confidence and ease.
4. Smart Snap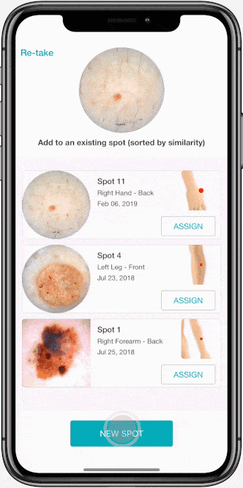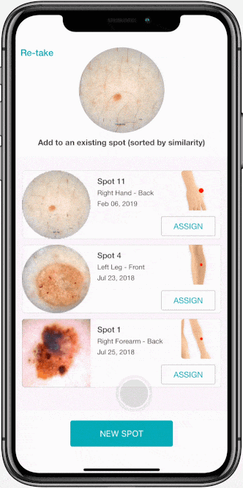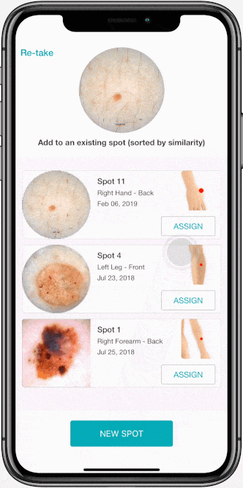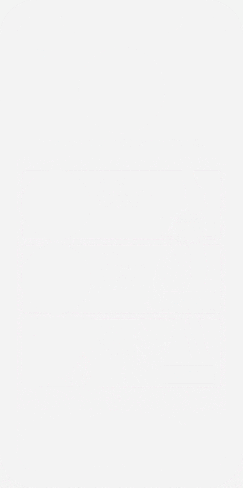
Which spot is from where? Certain patients have more spots than others, making it especially tricky to accurately capture follow up images of the correct lesion when there are no baseline photos, or they do not clearly indicate the placement of the spot. When in the middle of this predicament, suddenly the notes you jotted saying “fourth lesion on the right of the shoulder blade” do not seem so helpful when there are three other spots that fit this frustrating description.
When capturing a new dermoscopic image, Smart Snap identifies the key visual markers of a lesion and suggest to which spot profile it belongs. Rather than scrolling through dozens of pictures playing the “matching game”, this intuitive tool streamlines your imaging workflow by over 80%.
5. Visual Search (CBIR)Once the imaging and documentation process is complete, it’s time to analyze the lesion in question. To combat the growing dermatologist shortage, many GPs are managing a growing number of dermatology-related cases. Unfortunately, due to overwhelming numbers, lack of confidence and education in dermatology, still as many as 59% of new referrals to a dermatologist are for diagnosis.2
Using Visual Search, a GP can input the dermoscopic image of their current case into the system, where the algorithms will analyze the lesion and retrieve the most visually similar images from a library of pre-labelled pathology images. From here, the GP can review the images, gain new insights, and learn about the history of these visually similar cases and make a confident, evidence-based decision. Much like having a library at your fingertips, Visual Search acts as a clinical decision support tool to equip medical professionals with the information they need for a case.
Conclusion
Together, these five innovations are changing the way medical professionals execute their daily practice. In a field where the early detection of skin cancer can increase survival rates by as much as 83%, it is absolutely essential that care providers are equipped with the most advanced, intelligent, and efficient tools to support their workflows and, as a result, their patients.3 As artificial intelligence continues to learn and expand, many industry experts assert that it will become a “clinical assistant” to care providers; how will it enhance your services?
-The MetaOptima Team
Are you interested in staying at the forefront of intelligent dermatology? See how DermEngine's total body photography software can streamline your practices today by booking your demo!
Sources
Topics: Dermatology Artificial Intelligence Total Body Imaging Total Body Photography AI Artificial Intelligence in Dermatology AI In Healthcare Dermatology Software Full Body Imaging Total Body Photography Software